Cardiovascular Disease Management module

Introduction
The bestpractice Decision Support CVD Management module provides up to date clinical support for health professionals in managing patients’ cardiovascular disease. Recommendations for prevention and treatment of cardiovascular disease are made based on a person’s calculated cardiovascular risk. Much of the information required in making a risk assessment is pre-populated from the PMS allowing a health professional to rapidly determine Cardiovascular Risk. Recommendations for management are then customised for the condition and history of each patient.
Background
Cardiovascular disease (CVD) is the leading cause of hospital admissions and mortality in New Zealand. It is recommended that decisions on prevention and treatment of cardiovascular disease are based on the likelihood of a person having a cardiovascular event over five years. These cardiovascular events include heart attack, angina, stroke, peripheral vascular disease and heart failure.
This means treatment for CVD in New Zealand is no longer focussed on individual risk factors but on a person’s absolute cardiovascular risk. The CVD risk can be estimated using information on age, gender, blood pressure, total and HDL cholesterol, smoking, and whether or not a person has diabetes. From the mid 1990s paper-based CVD risk charts have been available in New Zealand to estimate peoples’ risk of having a cardiovascular event over five years. However these may have been under-used so a programme to increase risk assessment and management using internet-based clinical decision support systems has been developed.
How it works
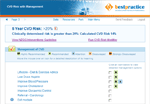
The BPAC Inc web-based Decision Support system calculates and displays a person’s absolute CVD risk then automatically saves it in a standard way to the patient’s medical record. This makes it superior to paper-based charts that can be interpreted in different ways, provide absolute cut-offs and require coding to a patients’ notes.
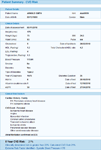
BPAC’s CVD Management uses data that is already in a patient’s medical record and the results of the latest routine assessment to determine the cardiovascular risk. It then automatically saves this in a standard way directly to the patient’s medical record.
Having calculated a person’s absolute CVD Risk, the bestpractice Decision Support CVD Management module lists the management options for each patient and the extent to which each would be recommended. These vary from Highly Recommended actions, i.e. those where failure to choose this action could strongly impact patient health, to Strongly Discouraged actions where choosing this action could impair patient health.
The bestpractice Decision Support CVD Management module makes recommendations based on the New Zealand Cardiovascular Guidelines Handbook 2009. These include the recommended interventions, goals and follow-up for each patient.
The module then facilitates this management as appropriate. For example, Lifestyle advice in the form of patient information leaflets, a pre-populated Referral form to Cardiology, the prescription of low dose aspirin or guidelines on management of risk factors such as cholesterol, blood pressure or glycaemic control.
Additional resources and tools are available to the user from directly accessible links or a drop-down menu. These include prescribing information from the British National Formulary (BNF), guidelines on Who to Screen and Frequency of Assessment. The references for the content of the module are listed and a selection of Frequently Asked Questions.
The New Zealand Guidelines Group Interventions Guideline is available already customised for the current patient, and the CVD Risk Tables can be viewed with the relevant value for this patient plotted. A unique tool is the CVD Risk Modifier which is a clear demonstration to patients of how their CVD risk will change as a person progresses towards their clinical targets.
Before concluding the CVD Management module, a Patient Summary is offered. Having read the CVD Risk information, a summary can be saved to the PMS with an option to print a copy if requested.
A patient recall is also offered before exiting the module with an automatic date default selected depending on the recommended bestpractice guidelines for each patient. For example, patients with 5-year CVD Risk >15%, diabetes, or on lipid or BP lowering medication, will be recommended to have an annual risk assessment and this can be set to occur through the usual PMS processes.
External Links
- New Zealand Cardiovascular Guidelines Handbook, 2009 Edition New Zealand Guidelines Group.
- Cardiovascular Disease Best Practice Journal, October 2008.
- What's New in the 2009 Cardiovascular Guidelines Handbook Best Practice Journal, June 2009.
Featured module

The INR Monitoring module utilises a formula developed by Ryan et al which assists clinicians adjust oral anticoagulant doses in patients. It also recommends the time interval for the next follow up visit and prints a Patient Dose calendar if required.
For more modules see the full list of standard modules.
Latest News
ACC18 Enhancements - Effective 27 November
Calendar, Printing and ACC Identifiers
In response to feedback, the online ACC18 continues to launch enhancements; the following will be available from 27 November.
Fitness for Work Tab - Calendar: Moving the mouse over the calendar for longer periods has been made easier.
Declaration Tab - ACC Identification: There will be a reduction in the number of identifiers from five to four; no direct impact on the Provider.
If you are one of the over 2000 Practitioners who regularly use the online ACC18; thank you. If you are not then now would be a good time to begin, noting that additional return to work assistance for patients is offered solely through this online form. Self service for setting up and using the online ACC18 is available at www.acc.co.nz (use keyword eACC18 Self Service). However, feel free to contact ACC at 0800 222 994 or ebusinessinfo@acc.co.nz for more personalised support.
Most Popular Modules
The five most popular modules in June were:
- Patient Prompt
- The Common Form
- e-Referral System
- ACC 18 Form
- CVD Quick Screen
To see more, go to the Statistics page.
Getting Started guide
The Getting Started guide is a good place to start if you are new to bestpractice Decision Support. The articles in the guide provide a quick and focussed introduction to the areas of most interest to new users of bestpractice.
About BPAC Inc
bestpractice Decision Support is produced by BPAC Inc. To find out more about us, click here.